Negotiating the M.H. System can be very confusing and intimidating. Often we may not understand how the system works, and may also not know our rights, which can lead to undesired situations and outcomes. In the interests of better understanding and enabling intelligent, informed decisions, we include some helpful info below in pdf’s to read and download; and relevant authorities to contact :


Flow Chart for Families to Understand the Steps Needed to Access
Intensive Behavioral Health Services (IBHS) June 2021 (pdf – infographic)
PA Mental Health Consent Law FAQ (pdf – infographic)
Overview of the PA Child Welfare System (pdf)
IBHS Acronyms (pdf)
PENNSYLVANIA LAW ON INVOLUNTARY COMMITMENT AND MENTAL HEALTH MANUAL; & PATIENT RIGHTS
Filing Grievances & Getting Help
- Every now and then, we find ourselves needing help. These are some resources:
- For all services in Butler County, covered by:
Beacon Health Options:
- Call 1- 877-331-7154
- Comsumers can file a complaint or grievance about any of their services or providers. For those services covered by Beacon Health Options, this is the phone# to call to file that grievance. The circumstances and events regarding the grievance will be noted and filed on your behalf. The grievance goes before the County and the oversight authority, Southwest Behavioral Health Management, Inc. See Brochure on How to get Help with a Health Choices Complaint and How Do I get Help with a Health Choices Grievance website http://sbhm.org/sw6.php
NAMI
- 724-431-0069
- NAMI may be able to provide you with helpful info in your situation
- To contact the NAMI HelpLine, please call 800-950-NAMI (6264), Monday through Friday, 10 a.m.–8 p.m., ET, or send an email to info@nami.org.
Butler County Human Services
- 724-284-5114 Leslie Johnson – Child
- 724-284-5114 Amy Cirelli – Adult
- Domestic Relations – 724-284-5181
Either the court or CYS can appoint a Guardian ad Litum to act in the interests of the minor.


MH/MR Program
Brandon Savochka, Human Services Director
124 West Diamond Street
Butler, PA 16003
724-284-5114
Marni Rettig – Mental Health Director
Butler County Human Services
124 West Diamond Street
Butler, PA 16003
724-284-5114
Pennsylvania Mental Health Consumers’ Association (PMHCA)
- Website: https://www.pmhca.org
- 717-564-4930 or 1-800-887-6422
- PMHCA@pmhca.org or Kathy Quick, Executive Director kathy@pmhca.org
- PMHCA is a state-wide member organization dedicated to the support of all people who seek aid for recovery from a mental illness at any stage in their journey. PMHCA provides resources, referrals, and support to those receiving services or in recovery from a mental illness.
Office of Mental Health & Substance Abuse Services (OHMSAS)
- P.O. Box 2675, Harrisburg, PA 17105-2675
- This office focuses on providing individuals who live with mental illness and substance use disorders with opportunities for growth, recovery and inclusion in the community, access to culturally competent services and supports of their choice, and a quality of life that includes family members and friends.
- Kristen Houser, Deputy Secretary Office of Mental Health & Substance Abuse Services
- OMHSAS Receptionist: 717-787-6443
- Phil Mader, Director Bureau of Community and Hospital Operations
Responsible for implementing and monitoring the community-based services and the unified service system initiative through collaboration with the county administrative offices. Also responsible for overseeing and directing the effective and efficient operations of the commonwealth-operated psychiatric hospitals (state mental hospitals) and South Mountain Restoration Center
- Kendra Snuffer, Chief of Staff
Responsible for coordinating the supervision of all office program components and special initiatives to improve and/or modernize services provided. Serves as a key member of the executive team, working with the deputy secretary to identify, emphasize, discuss and resolve issues impacting services. Establishes goals and objectives to implement the office’s strategic plan; develops and implements policies and procedures; and provides leadership and coordination to office program managers to ensure that all programs are providing high-quality services.
- Dr. Dale K. Adair, Medical Director
Serves as Chief Medical Officer for the state mental hospital system, and as Chief Clinical Officer with oversight of the HealthChoices program. HealthChoices is a managed care program currently covering more than 70 percent of the medical assistance enrollees across the commonwealth. The medical director leads quality assurance activities and directs clinical programming by implementing “best practices” in clinical psychiatry and addiction treatment for the hospitals.
- Jamey Welty, Director Bureau of Policy, Planning & Program Development
Responsible for performing a full range of planning and developmental functions — these include managed care design and development, service system design and development, policy and program development, state and county planning, and human resource development within OMHSAS.
- Scott Talley, Director Bureau of Children’s Behavioral Health Services
Responsible for the policy, program, and operations of the Children’s Behavioral Health delivery system. The Bureau of Children’s Services promotes the emotional well-being of children and ensures that children with emotional disorders live, learn, work, and thrive in their communities.
- Amanda Roth, Director Bureau of Quality, Data and Clinical Review
Responsible for the development, oversight, and direction of the quality management program. Also responsible for associated data management and data reporting functions. The Quality Management program provides the framework for OMHSAS to assess and improve the quality of publicly funded behavioral health administrative services, clinical systems, and clinical care. Oversees management and execution of Medicaid provider functions and PROMISe system for behavioral health services. Oversees operation of Medicaid fee for service (FFS) authorization processes.
- Kellie Mainzer, Director Division of Western Operations
Piatt Place, 301 Fifth Avenue, Room 480, Pittsburgh, PA 15222 - Southwest Field Office: 412-565-5226
- kmainzer@pa.gov
Responsible for oversight of mental health and drug and alcohol services in 47 western region counties. Directs the operations of the Harrisburg and Pittsburgh field offices. Offices are responsible for licensure, county plan review, HealthChoices oversight, and day-to-day county government interface

Child Abuse, Trauma & Toxic Stress and the Effects on Children and Young Adults.
Long Term Consequences of Child Abuse & Neglect (pdf)
Toxic Stress & Adverse Childhood Experiences (ACE’s) (pdf – infographic)

A Cause for Concern
- Coercive Psychiatry by David Oakes (click on link to read pdf)
- The Moral Imperative for Dialogue with Organizations of Survivors of Coerced Psychiatric Human Rights Violations
- David Oakes, the Director of the NGO Mind Freedom International, personally experienced coerced psychiatric procedures in a variety of ways over a three-year period as a young adult. He was thus motivated to become a community organizer in the field of human rights in mental health. He considers the coerced psychiatric procedures he was subjected to as significant violations of his human rights that profoundly traumatize him to this day. In his 25 years as director of Mind Freedom International, he testifies that
- “… nearly every day our office receives new, moving, poignant, personal reports of abuse in the contemporary psychiatric care system, usually related to some type of coercion.“
- “The types of abuse I hear about have continued unabated throughout all these years, to the present time. My subjective perception is that this psychiatric coercion is increasing, and in fact appears to be expanding rapidly into poor and developing countries.”

Know Your Medications

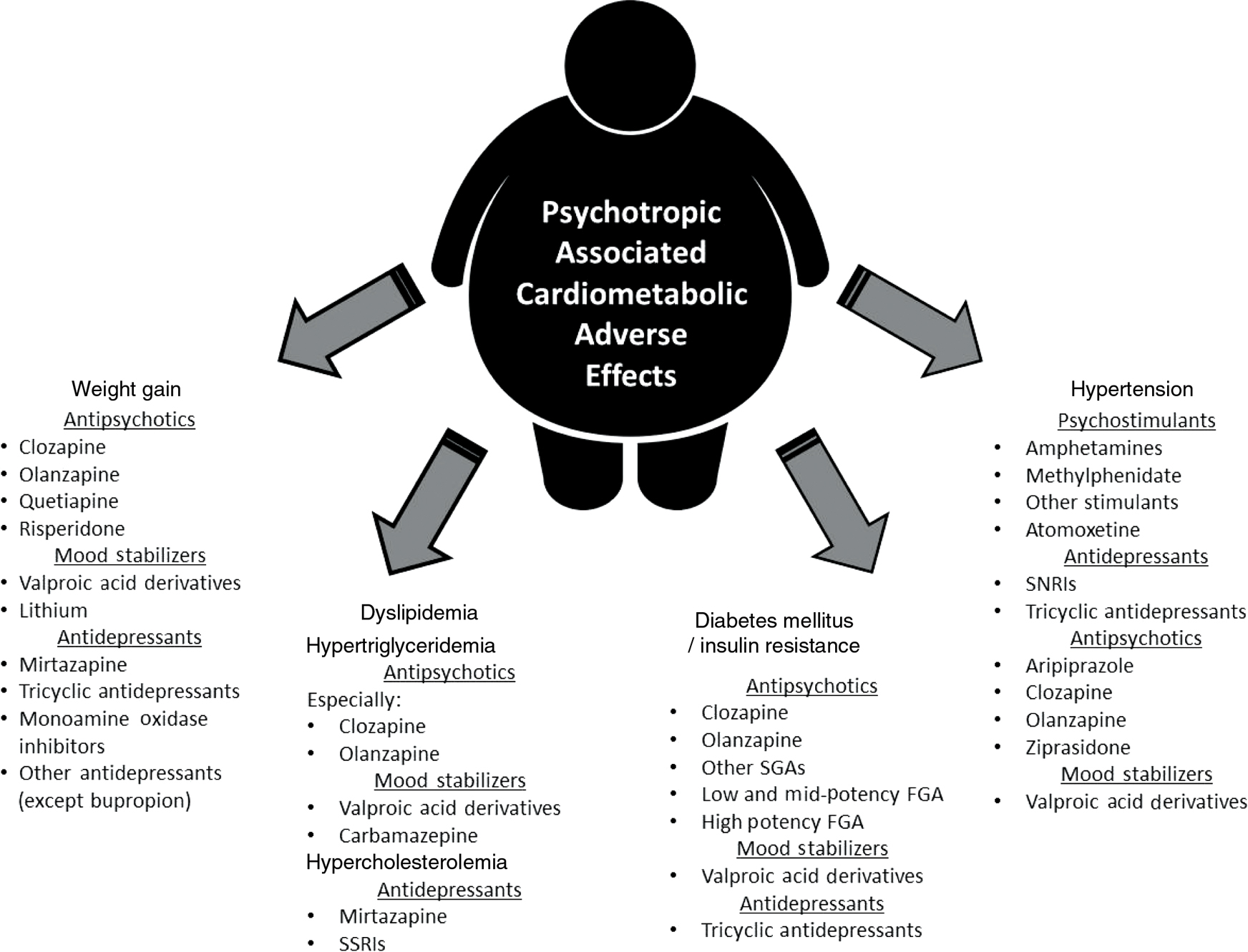
What is a Psychotropic Drug? (click on link to read pdf)
A Guide to Common Antidepressant Side Effects (click on link to read pdf)


Take The ACE Quiz for your Life — And Learn What It Does And Doesn’t Mean
Ethics and Mental Healthcare
As mental health clients, we may have heard a word from providers called ethics.
What is ethics? Ethics are a set of moral values relating to a specific group, field or form of conduct. In some ways, it is about being moral and behaving in the right way.
The legal parts of client care are controlled by regulations which are ruled by ethics. For example, if a counselor is said to have done something wrong, it must be made certain he or she acted against ethics or laws. Ethics must help guide those who are involved in moral issues. Good ethics must be clinically relevant. Providers are guided by ethics. Ethics such as:
- Privacy
- Confidentiality
- Maintaining limits
- Individual and cultural understanding
- Professional
Mental health providers face ethical problems that are difficult. When a client’s mental health is at risk, can rights such as personal freedom be challenged? A client may share personal information with their provider. Clients often find themselves in vulnerable positions where the provider has the power. This can result in boundary violations.
Compassion is an important part of being a professional. So are transparency, honesty, listening to the client and respecting the basic human rights of the client. A mental health provider must always act in a manner that demonstrates the highest values of his profession and value the trust put in him by the client.
Source: McMillan J. Good medical ethics. J Med Ethics. 2018;44:511–2. [PubMed] [Google Scholar] 2021 Beacon Health Newsletter


